A Simple Test, A Powerful Step Toward Prevention.
A colonoscopy is a medical procedure used to examine the inside of the colon (large intestine) and rectum using a long, flexible tube with a camera on the end. It allows doctors to detect abnormalities such as polyps, inflammation, ulcers, or cancer, and even treat certain conditions during the procedure.
Colonoscopy can detect precancerous polyps before they turn into cancer. These growths can often be removed immediately during the procedure, reducing the risk of colorectal cancer.
For patients with ulcerative colitis or Crohn’s disease, colonoscopy provides detailed images to assess inflammation, damage, and disease activity. Biopsies can also be taken to guide treatment.
Bleeding from the rectum can be caused by hemorrhoids, diverticulosis, polyps, or cancer. A colonoscopy can identify the source and allow for real-time intervention.
Persistent bowel habit changes may signal underlying structural or functional problems, which colonoscopy can help evaluate and treat.
Unexplained anemia could be a sign of slow internal bleeding in the colon, especially in older adults. Colonoscopy is often recommended to rule out bleeding polyps or cancers.
1. Sedation
Before starting, you’ll be given sedation through an IV line. This medicine makes you feel calm, relaxed, and comfortable. Most patients don’t feel any pain and often don’t remember much about the procedure.
2. Insertion of the Colonoscope
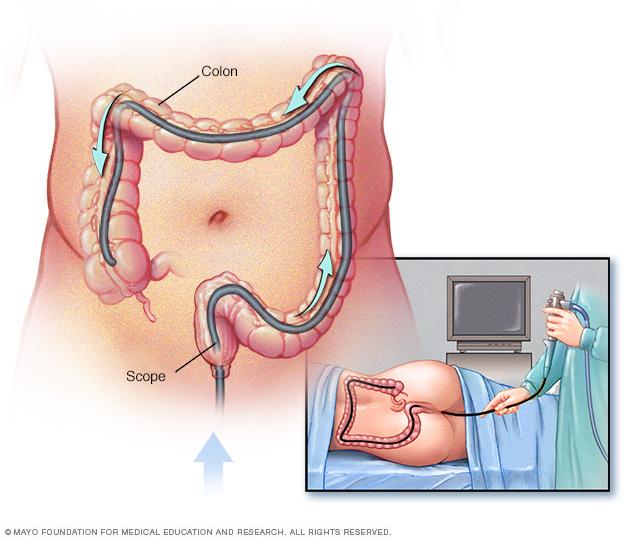
Once you are comfortable, the doctor gently inserts a thin, flexible tube called a colonoscope into your rectum. This tube has a small camera and light at its tip, which sends real-time images to a monitor, helping the doctor see the inside of your colon clearly.
3. Careful Examination
The doctor slowly advances the scope through the colon, carefully examining the lining for any polyps (small growths), inflammation, ulcers, bleeding, or other abnormalities.
4. Polyp Removal or Biopsy (if required)
If the doctor finds polyps, they can be removed right away during the same procedure. In some cases, a small tissue sample (biopsy) may be taken for further laboratory testing. This is a routine part of the exam and is usually painless.
5. Duration of the Procedure
The entire colonoscopy typically takes 20 to 60 minutes, depending on whether polyps are removed or biopsies are taken.
6. Recovery
After the exam, you’ll be moved to a recovery room while the sedation wears off. Most people feel drowsy or lightheaded for a short time but recover fully within 1–2 hours. You’ll need someone to accompany you home, as you should avoid driving or operating machines for the rest of the day.
To get clear images, your colon must be completely clean:
You’ll follow a clear liquid diet for 24 hours
A bowel prep (laxative solution) is taken the night before and possibly the morning of the exam
Fasting is required after midnight
Sedation is administered to help you relax
The colonoscope is gently inserted through the rectum
The doctor examines the lining of the colon and may remove polyps or take biopsies
The entire procedure takes 20 to 60 minutes
You’ll rest in a recovery area until the sedation wears off
Mild abdominal cramping
Bloating or gas
Sore throat (if sedated through mouth)
These typically go away within hours.
Perforation of the colon wall (~1 in 1,000 cases)
Bleeding, especially after polyp removal
Reaction to sedation
Infection (extremely rare)